This post is written and sponsored by Overland Park Regional Medical Center. When your child is sick or injured, trust the expertise of The Pediatric Center at Overland Park Regional Medical Center to get them back to being a kid again. To learn more about The Pediatric Center and meet our pediatric specialists, visit hcamidwest.com/pediatrics.
I was having a very healthy pregnancy until 32 weeks when I started feeling extremely nauseous and fatigued to the point that I got dehydrated. I could not keep anything down. Initially, I put it off as just last trimester nausea, but as I look back now I whole-heartedly believe my body was trying to tell me that there was something seriously wrong with my pregnancy.
I had noticed that my baby had not been as active as she usually was. I did everything I could think of to get her to move, from drinking a soda to laying a specific way. I knew something was wrong and decided to go to the local hospital in Joplin, Missouri. At this time we had about six inches of snow on the ground, which made our trip to the hospital a little longer than usual. When we arrived at the hospital, I was immediately taken up to the Labor and Delivery Unit where they hooked me up to monitors. I felt immediate relief when they found her heartbeat. At this point, I thought they would just monitor her for a few hours and send us home. What I did not know was that she was having decels, which are temporary decreases in the fetal heart rate during labor. I was told it was a sign that the baby wasn’t doing well, and this was very concerning to the doctors.
A few hours after monitoring her heart rate, they sent in an ultrasound tech who performed a biophysical portfolio, or BPP, which measures a baby’s heart rate, muscle tone, movement, breathing and the amount of amniotic fluid around the baby. She only scored 4/10, causing even more concern that something was seriously wrong. A high-risk OB team from Overland Park Regional Medical Center nearly 150 miles away was notified and used telemedicine to evaluate my baby and me. Another ultrasound and a more in-depth BPP was performed, and our baby girl scored poorly with a 4/8. At this time, they also discovered that she had a dilated loop of bowel, causing a blockage in her bowels, and the doctors felt that this was why she was getting sick.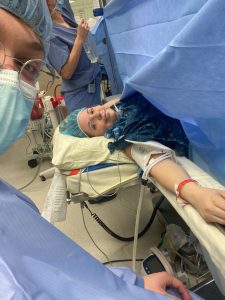
The medical team at Overland Park Regional Medical Center, along with my team in Joplin, decided that it was best for my baby and me to be transported to the antepartum unit at Overland Park Regional Medical Center where a pediatric surgeon and a neonatal team could take care of me and our baby girl. Because her condition was so serious, the Maternal Transport Team from Overland Park Regional Medical Center brought me to the hospital in Overland Park, Kansas, via helicopter. After arriving at Overland Park Regional Medical Center, the labor and delivery team performed another BPP ultrasound, and this time she scored 2/10. I was told that I would have to deliver by an emergency cesarean section. My husband had to travel by car, so while he was on his way I was prepped for the C-section. Upon his arrival, we were immediately taken to the operating room for the delivery.
In the operating room, there was an entire medical team to take care of me, but there was also another entire medical team just to take care of my baby. Ophelia Mae was born weighing 4 pounds, 4 ounces. Ophelia was very pale, she was not breathing, and her heart rate was too slow. She was quickly given to the neonatal team and they all went to work to save our baby girl. She was given oxygen and an IV. Then a special tube, called a replogle, was placed to empty her stomach and bowels, which relived the pressure on her heart and lungs. After 10 minutes, she began breathing regularly and her color began to improve. Ophelia was immediately transferred to the NICU where they began running tests and getting X-rays, including a contrast enema to get a definite diagnosis of what was going on with her bowels. I was so grateful that Ophelia and I were able to be together and she was not whisked away to another hospital. She was just one floor above me, and I got to see her once I felt better.
 We met our Pediatric Surgeon, Dr. Corey Iqbal, and he explained Ophelia’s diagnosis and treatment plan. It was such a scary time, but Dr. Iqbal explained everything in a way that my husband and I would understand, which answered all of our questions before we even had to ask them. My husband and I are young parents, so we are very inexperienced when it comes to things of this nature. We were devastated at the thought of our baby going through so much at the beginning of her life. Four days after Ophelia’s birth, Dr. Iqbal performed surgery and found an ileal atresia, which is when a part of the bowel does not completely develop resulting in a blockage. It was explained to us as a congenital condition, which means it develops before birth. In Ophelia’s case, the blockage had also caused a twist in her bowels, which was making her sick in the womb. The twist was also cutting blood flow to other parts of Ophelia’s bowels. Dr. Iqbal removed nearly one-third of Ophelia’s small bowel and placed an ostomy bag, which is a temporary way to control problems with bowels when babies are so small and gives them a chance to recover from surgery. He also created a mucous fistula, which was a second ostomy that allowed the NICU nurses to re-feed anything from the ostomy bag back through Ophelia’s bowels to allow her to eat and keep her bowels fully functional during her recovery, which would be several weeks.
We met our Pediatric Surgeon, Dr. Corey Iqbal, and he explained Ophelia’s diagnosis and treatment plan. It was such a scary time, but Dr. Iqbal explained everything in a way that my husband and I would understand, which answered all of our questions before we even had to ask them. My husband and I are young parents, so we are very inexperienced when it comes to things of this nature. We were devastated at the thought of our baby going through so much at the beginning of her life. Four days after Ophelia’s birth, Dr. Iqbal performed surgery and found an ileal atresia, which is when a part of the bowel does not completely develop resulting in a blockage. It was explained to us as a congenital condition, which means it develops before birth. In Ophelia’s case, the blockage had also caused a twist in her bowels, which was making her sick in the womb. The twist was also cutting blood flow to other parts of Ophelia’s bowels. Dr. Iqbal removed nearly one-third of Ophelia’s small bowel and placed an ostomy bag, which is a temporary way to control problems with bowels when babies are so small and gives them a chance to recover from surgery. He also created a mucous fistula, which was a second ostomy that allowed the NICU nurses to re-feed anything from the ostomy bag back through Ophelia’s bowels to allow her to eat and keep her bowels fully functional during her recovery, which would be several weeks.
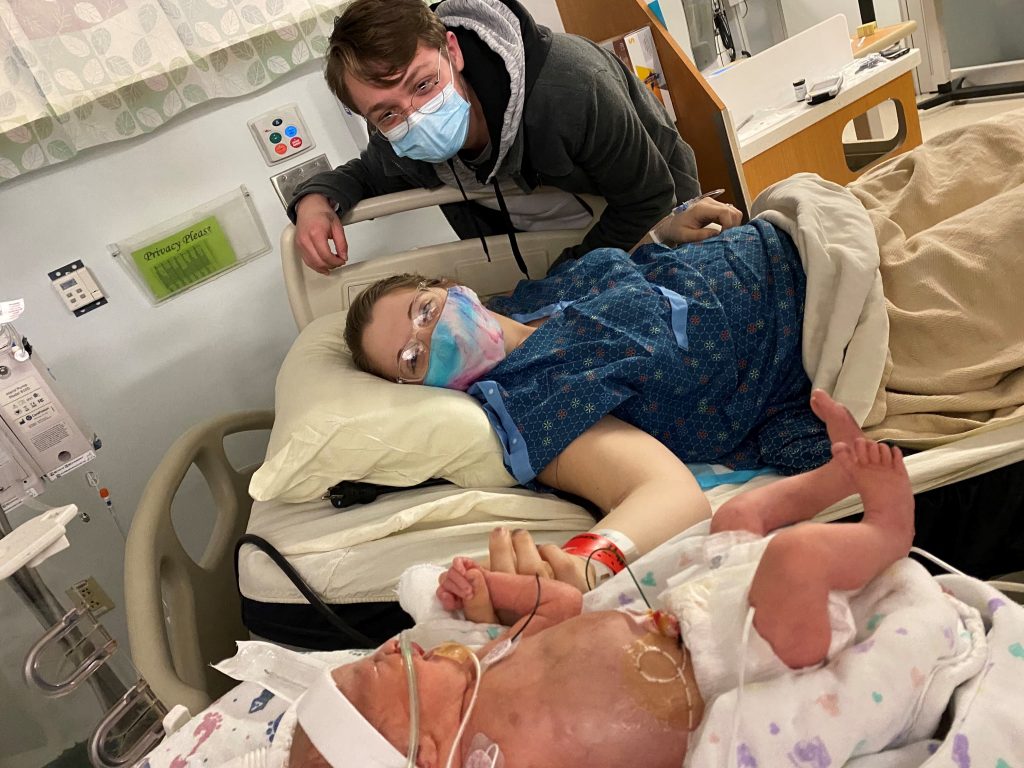
When we first saw Ophelia after her surgery, we were absolutely amazed at how such a tiny human could go through what she had just went through, but so thankful to see she was OK. We were determined to do everything we could to help Ophelia on her journey. Ophelia spent six weeks in the NICU with her ostomy bag before Dr. Iqbal performed a reanastomosis where he was able to reconnect her bowels and leave minimal scarring to her abdomen. This was a complete miracle! 
Ophelia had a bowel movement the night of her reanastomosis surgery, which surprised everyone. We started her feedings just two days later, and she ate like a champ! The team quickly decided we could start increasing her feeds. We were at full feeds within four days, and she started having regular bowel movements immediately. Thanks to Dr. Iqbal and the amazing NICU team, Ophelia graduated from Overland Park Regional Medical Center’s NICU at 8 weeks old.
The NICU and pediatrics teams at Overland Park Regional Medical Center made our journey a lot less stressful than what it could have been. They supported and guided us through something that neither my husband nor I could have ever expected. Ophelia is now 12 weeks old and is close to 9 pounds! She is fully healed and is as healthy as any baby her size. We were so happy to finally introduce Ophelia to her older sister, and we are so excited to say that her sister is just as in love with her as we are. We are forever thankful to Overland Park Regional Medical Center for taking such great care of our family.
 Ambe Nelson lives in Joplin, Missouri, with her husband and two daughters.
Ambe Nelson lives in Joplin, Missouri, with her husband and two daughters.
















